What's the difference between Post Acute Sequelae of COVID-19 (PASC) and mRNA COVID-19 Vax Injury?
Implications for Therapy
IMAGE 1. From Patterson et al, 2022 (preprint)[1].
From a large study [1], involving 236 (USA) patients comprising:
64 with PASC
50 with ME-CFS
29 with Lyme disease
42 with Post-Vax (with PASC overlapping signs and symptoms)
26 with mild-moderate acute COVID-19 (MM), and
25 with severe acute COVID-19 (Severe)
Patterson et al, were able to derive a classification system to distinguish the above disorders from each other based on a hierarchy of cytokine levels (IMAGE 1).
There were no cases of sudden death studied for obvious reasons.
Here is my interpretation of IMAGE 1.
That the algorithm starts with GM-CSF suggests that M1-like macrophages are the primary response affected in the various post-infectious responses which I do believe to be true [2].
On the right are diseases that primarily involve innate immunity (MM and ME-CFS).
On the left with the involvement of IL-2 there are both adaptive and innate immunity components.
For the GM-CSF - CCL5 - TNF-alpha -IFN-gamma characteristic of ME-CFS symptoms/disease; we know it is the CCR5 monocytes in peripheral blood (CCR5 is the receptor for CCL5 [3]) which comprise the intermediate monocytes (Mono_C4-CD14-CD16 [4]) that develop into the lipid body negative foamy macrophages (Macro_c5-WDR74 [4]) that produce high levels of the potent protector HERV-K102 particles [2].
In the bronchoalveolar lavage fluids (BALF) of moderate COVID-19 patients, there are only 2 cell types of the 63 different populations of cells which exhibit HIGHLY activated vitamin D receptor regulons: the macrophages that produce HERV-K102 particles and their progenitors, the intermediate monocytes [4]. As explained elsewhere the M1-like foamy macrophages that produce and release the HERV-K102 particles by lysis are ESSENTIAL for prevention of or recovery from, COVID-19 [2]. Also systematic reviews and meta-analysis have revealed optimal levels of Vitamin D3 strongly protect against SARS-COV-2 symptomatic infection, severe COVID-19, death from COVID-19 and even all-cause mortality more generally [5] consistent with Vitamin D3 promoting production of the HERV-K102 protector particles and/or preventing SARS-COV-2 mediated immunosenescence of macrophages that causes chronic diseases like cancer, cardiovascular diseases, increased susceptibility to infections and so on.
The steadfast production and release of the protector HERV-K102 particles from foamy macrophages when confronting SARS-CoV-2 seems highly dependent on optimal serum levels of vitamin D3 (Image 2)[2].
IMAGE 2. Vitamin D3 over 50 ng/ml prevents onset of severe COVID-19.
Since the release of the HERV-K102 particles is by lysis, this means the body must continuously cause bone marrow progenitors to develop along the intermediate monocyte then M1-like macrophage pathway… explaining the critical involvement of elevated GM-CSF in the post-infection syndromes.
It also explains why in a large study of PASC patients, the intermediate monocytes in peripheral blood were significantly elevated over normal healthy controls [6]. For non-immunologists, it should be appreciated that generally there are no macrophages in the blood, except in severe/critical COVID-19 [4] which could represent emergency myelopoiesis.
Chronic fatigue syndrome (CFS) involves fatigue, insomnia and brain fog which apparently associates with very high levels of HERV-K102 particle production and lytic release. St. John’s wort in vivo blocked fatigue, insomnia and brain fog in a CFS patient associated with the 100 % inhibition of HERV-K102 cDNA production in plasma [6,7]. In contrast by 84 hours off therapy there were 2.55 × 10(11) cDNA containing particles per ml of plasma showing a dramatic RAPID increase in HERV-K102 particle release/production [7]. St. John’s wort (hypericum) was also shown to block HERV-K102 replication in vitro (IMAGE 3).
IMAGE 3. St. John’s wort blocks HERV-K102 cDNA (particle) production in vitro.
Here, the ddCt real time qPCR for HERV-K102 polymerase (pol) is compared to 18 S RNA gene that controls for amount of genomic DNA present. The ddCt values exceeding the unincubated PBCs (day 0) ratio of 0.77 indicates and excess signal of pol in genomic DNA and/or cDNA associated with the HERV-K102 particles. To identify an increase in genomic integration such as associated with low dose tuftsin (known to activate macrophages while high dose inhibits) the assay is repeated in the presence of UNG which digests the cDNA of particles leaving the genomic DNA for analysis. Here all analyses were performed on isolated DNA. So the data shows that in the case of low dose tuftsin, there was an almost 3 fold increase in HERV-K102 proviral copy number. So not only does HERV-K102 replicate in vitro in this media (but not other medias like RPMI) but as expected, it involved integration known to be involved in retrovirus replication.
Accordingly, CFS with its insomnia, fatigue and brain fog, might be characterized by persistent activation of HERV-K102 in the foamy macrophages which is induced by TNF-alpha and IFN-gamma as well as other mediators [2].
That patients with mild or moderate COVID-19 also align with the CFS type patients, shows there is no interference of the innate immunity HERV-K102 response of foamy macrophages when there is no spike IgG1/3 made prior to clearance of SARS-CoV-2 by innate immunity.
The GM-CSF to CCL5 and TNF-alpha might signify the early recruitment and activation of the CCR5 positive intermediate monocytes [2] in mild and moderate COVID (MM).
As we move left in Image 1, the involvement of IL-2 indicates the involvement of adaptive immunity in the pathology of these post-infection syndromes.
The response featuring IL-4 (the TH2 mediated antibody response) is associated with the Post-vax syndrome. After the second shot of the mRNA vaccines, IgG1/3 antibodies to spike are made and cause SARS-CoV-2 particles to enter the protector foamy macrophages by antibody dependent enhancement (ADE) of infection into macrophages [2 and see IMAGE 2 above].
PASC itself likely involves the persistent activation of HERV-K102 which relates to elevated IFN-gamma [2] which is also found in ME-CFS. However in PASC, the antibodies to spike protein (ie., influenced by IL-4) induce immunosenescence of macrophages which allegedly distinguishes it from ME-CFS.
Soluble CD40 ligand (sCD40L) derived from activated platelets is immunosuppressive to macrophages and indicates a prothrombotic (hypercoagulation) state. It blocks monocyte activation and activates the myeloid dendritic cells to induce active immunosuppression by way of the T regs. Interestingly, sCD40L is elevated in association with metastasis and the progression of cancers [9] in addition to post-COVID vax injury and more severe COVID-19.
The combination of IL-13 with IL-4 is involved with Type 2 antibody responses and plays a role in wound repair [9]. They suppress initial inflammatory responses and control how extracellular matrix is modified during wound repair [9].
There may be a subtype of post-vaccination patients where there is hypercoagulation (the COVID-19 vaccines are sometimes referred to as the clot shots).
Presumably, patients with ‘turbo cancer’ would fall in with the severe C19 category as these have been characterized as having a high neutrophil to lymphocyte ratio (at 3+ where normal is around 2) [11] and where IL-8 (CXCL8) attracts and induces neutrophil activation [12]). Note also that glucocorticoid resistance (a feature of severe COVID-19 and malignant cancers [13]) is associated with a hub involving myc, CXCL8 (IL-8) and ATF3 where LCN2 is downregulated [13]. LCN2 upregulation is needed for apoptosis such as for release of the HERV-K102 particles by the lysis of sebocytes [14] which are specialized M1-like, lipid body negative foamy macrophages. Probably its downregulation in association with CXCL8 would be associated with strong immunosenescence of macrophages related to severe COVID-19 and ‘turbo cancers’. Thus, CXCL8 (also known as IL-8) [12] would be related to risk of high mortality. Interestingly in 90 year olds, the expression of HERV-K102 transcripts in PBMCs is associated with CXCL8 but not in younger adults [15].
More recently, Patterson et al have performed a case series where the combined use of a CCR5 chemical antagonist, maraviroc along with pravastatin for 6 to 12 weeks was shown to improve various clinical scores in 18 PASC patients along with changes to a number of cytokines outlined in Image 1 [16]. This regime would block the activation of monocytes/macrophages.
Aside from the hypercoagulation associated with spike protein and SARS-CoV-2 infections, immunosenescence involving immunosuppression and paradoxically also inflammation [17, 18] would be more dangerous than immunosuppression alone because the former exacerbates chronic diseases like cancer and cardiovascular diseases. Accordingly, there may be some merit in using anti-inflammatories to help resolve some of the symptoms of PASC or post-vax syndromes (to my own chagrin).
On the other hand, the loss of immunosurveillance against cancer and infectious agents by using immunosuppressive drugs (categorized as anti-inflammatories. like statins) particularly in the aged, to me would invite disaster. I do believe alpha-fetoprotein (AFP) antagonists which reverse immunosenescence (like vitamin D3, zinc, ivermectin [19], 7-keto-DHEA, genistein/isoflavones and possibly now artemisinin) are the way forward not only for the treatment of PASC, post-vax syndrome, ‘turbo cancer’ and others but should be employed as the first line of therapy to deal with any emerging pathogen or the feared ‘X pandemic’.
It remains to be determined if the failure to resolve post-vax syndromes and PASC in patients has to do with the common inclusions of anti-inflammatories used in the first line of therapy in PASC patients.
Note however that methylprednisolone works well against severe COVID-19 (but not so much dexamethasone) [20]. Although both corticosteroids are classified as anti-inflammatories, it seems possible the former might actually induce HERV-K102 particle production but not dexamethasone [2]! (This needs to be investigated and validated asap). This may be why low dose methylprednisolone doesn’t seem to interfere with SARS-CoV-2 clearance [21].
Because glucocorticoid resistance is an important component of severe COVID-19 and ‘turbo cancers’ I would strongly recommend reading a review article by Dr. G. Umberto Meduri and GP Chrousos [22]. This comprehensive document details how the immunosenescence of macrophages [17,18] that they called Persistent Inflammation, Immunosuppression and Catabolism Syndrome (PICS) involves blocked glucocorticoid receptor signaling which underlies chronic disease. This PICS/immunosenescence pre-condition plays a role in susceptibility to acute respiratory distress syndrome (ARDS), such as in severe COVID-19 or sepsis patients.
In my opinion, it would be best to completely avoid all agents capable of blocking macrophage activation to ensure the production (and release) of HERV-K102 particles. This would also include the contraindication of plant based amino acid supplements where the higher ratio of arginine to lysine would block macrophage activation in part by lowering available cholesterol needed for high HERV-K102 particle production [23] (and which is similar to statins).
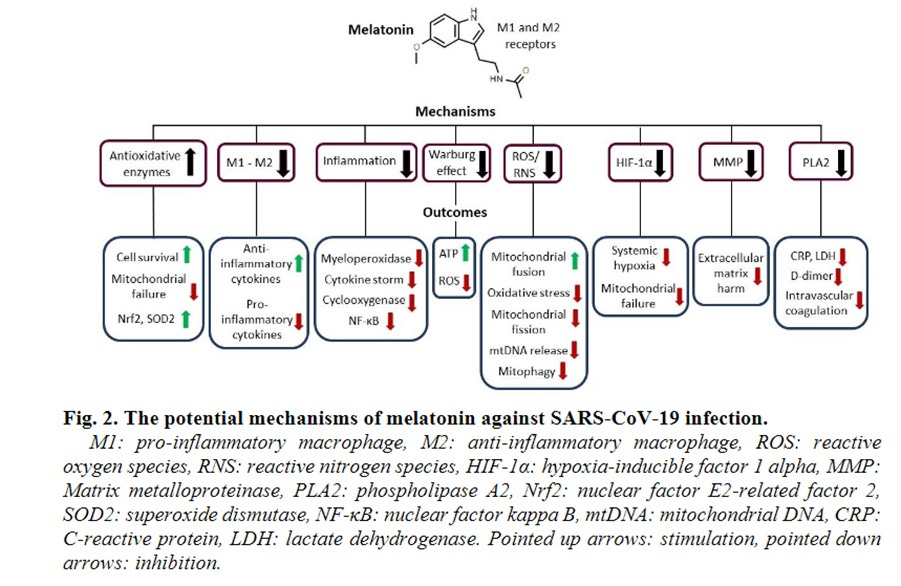
Melatonin (at high dose > 2 mg per night) has been recommended for the treatment of patients with PASC/cancer. The problems with melatonin is that when it is given at doses higher than 2 mg per night, it immunosuppresses the M1 like proinflammatory foamy macrophages. There is evidence it converts these protector macrophages to non-protector [24] by converting them to M2-like foamy macrophages (Images 4 and 2) .
IMAGE 4. From [24].
Indeed recent evidence suggests near infrared exposures can cause the mitochondria to produce melatonin which since it is an anti-oxidant would be sufficient to compensate for reactive oxygen species generated when energy production is derived from glycolysis in the M1 like proinflammatory macrophages [25]. In other words, provided one gets near infrared exposures there is already plenty to go around.
Finally, recent evidence shows melatonin may have variable or perhaps even unpredictable effects on cancers [26] as demonstrated in IMAGE 5.
IMAGE 5. Melatonin Affects Cancer Pathways Inconsistently Across the Board [26]
Proposed Therapy for PASC, Post-Vax Injury, ‘Turbo Cancers’ and Potentially Shedding
If the source of S1 spike protein in the non-classical CD16+ monocytes of blood samples of PASC (demonstrated in 73% of cases or 19/26 [27]) is not due to transfection of gut bacteria with the vaccinal spike mRNA (via direct vaccination or by shedding from the vaccinated), a better approach to resolve PASC, Post-Vax Injury, and/or ’turbo cancer’ might be to treat these patients with methylprednisolone plus the above mentioned AFP antagonists that would block immunosenescence/PICS. Since AFP antagonists would reverse apoptosis resistance and allow for the lytic release of the HERV-K102 particles from the foamy macrophages, at the very least this would remove the dysfunctional macrophages and the failed glucocorticoid receptor signaling [22]. At the same time, this would reinstall the potent immunosurveillance against tumors and infectious agents/toxins of the M1 like pro-inflammatory foamy macrophages (see Image 2).
Critically, the ingestion of any “anti-inflammatory drug (especially statins), herbal medicines (turmeric and perhaps most herbal medicines) and melatonin over 2 mg per night” should be contraindicated largely because they prevent the production and/or release of HERV-K102 protector particles needed for recovery and moreover, do not remove the dysfunctional macrophages causing the problems.
Nattokinase and bromelain should be used to digest any spike protein such as in the gut and/or involved in the risk of clotting. Replenishing any vitamin deficiencies also would be advised and the use of anti-oxidants [22] (vitamin C, NAC and near infra-red exposures) should be encouraged to enhance the speed of recovery.
In recognition that there could be transfection of gut bacteria with the vaccinal spike mRNA in the directly vaccinated and possibly by shedding to the unvaccinated, high dose pre-and pro-biotics should also be taken as part of the therapy and continued indefinitely (until no SARS-CoV-2 circulates globally and the mRNA vaccines are banned outright).
I have previously written on how to distinguish turbo cancers [https://hervk102.substack.com/p/how-to-distinguish-turbo-cancers] as well as discussions implicating the SV40 contaminants of the Pfizer vaccines in promoting very rapid progression of cancers [https://hervk102.substack.com/p/on-the-subject-of-turbo-cancers] which may be of some interest to some readers.
I have also provided some preliminary evidence consistent with adverse effects of shedding from the recently vaccinated (especially around the time of the emergence and dominance of the delta variant coincident with the administration of the second dose in elder populations, see B > C in Image 6). Allegedly, this might increase C19 and non-C19 mortality in the unvaccinated [https://hervk102.substack.com/p/attempts-to-quantify-impact-of-shedding] as summarized in Image 6 B & C.
However, the good news from Image 6 is that (presumed uncontaminated) HERV-K102 particle shedding from the upper respiratory tract such as when activated by the first dose of the COVID-19 vaccine (see A in Image 6) seems to horizontally spread protection to the unvaccinated decreasing both C19 and non-C19 mortality. NOTE A is without the ADE promoting spike IgG1/3 in the URT found with the second dose B [2].
A better and safer approach would be to use non-gene therapy and non-adaptive vaccines such as the Kleen et al, IMM-101 innate immunity vaccine developed by Professor Angus Dalgleish [28].
So there would be hope moving forward for enhanced establishment of (sterilizing) herd immunity with innate immunity vaccines including the horizontal protection of the yet uninfected and unvaccinated by putatively activating HERV-K102 particle production shedding.
IMAGE 6. UK ONS mortality rate data suggesting shedding of HERV-K102 particles to the unvaccinated can reduce (A) or increase (B) mortality rates in the unvaccinated.
But for the most part, ensuring optimal levels of vitamin D3 (Image 2) along with early treatment with the protocol discussed here would be expected to keep the vulnerable out of the hospital for any emerging pathogen or the onset of Pandemic X.
REFERENCES
Patterson BK et al., Cytokine Hub Classification of PASC, ME-CFS and other PASC-like Conditions, Research Square Preprint April 2022, DOI: https://doi.org/10.21203/rs.3.rs-1598634/v1.
Laderoute, M. Antibody Dependent Enhancement (ADE) of Infection into Macrophages Validates the Importance of HERV-K102 Particle Production for Pandemic Preparedness. Preprints 2023, 2023120185. https://doi.org/10.20944/preprints202312.0185.v1.
Chernov AS, Rodionov MV, Kazakov VA, Ivanova KA, Meshcheryakov FA, Kudriaeva AA, Gabibov AG, Telegin GB, Belogurov AA Jr. CCR5/CXCR3 antagonist TAK-779 prevents diffuse alveolar damage of the lung in the murine model of the acute respiratory distress syndrome. Front Pharmacol. 2024 Feb 21;15:1351655. doi: 10.3389/fphar.2024.1351655.
Ren X, Wen W, Fan X, et al. COVID-19 immune features revealed by a large-scale single-cell transcriptome atlas. Cell. 2021 Apr 1;184(7):1895-1913.e19. doi: 10.1016/j.cell.2021.01.053.
Gomaa AA, Abdel-Wadood YA, Thabet RH, Gomaa GA. Pharmacological evaluation of vitamin D in COVID-19 and long COVID-19: recent studies confirm clinical validation and highlight metformin to improve VDR sensitivity and efficacy. Inflammopharmacology. 2024 Feb;32(1):249-271. doi: 10.1007/s10787-023-01383-x.
Patterson BK, Guevara-Coto J, Yogendra R, Francisco EB, Long E, Pise A, Rodrigues H, Parikh P, Mora J, Mora-Rodríguez RA. Immune-Based Prediction of COVID-19 Severity and Chronicity Decoded Using Machine Learning. Front Immunol. 2021 Jun 28;12:700782. doi: 10.3389/fimmu.2021.700782.
Laderoute MP, Giulivi A, Larocque L, et al. The replicative activity of human endogenous retrovirus K102 (HERV-K102) with HIV viremia. AIDS. 2007 Nov 30;21(18):2417-24. doi: 10.1097/QAD.0b013e3282f14d64.
Laderoute MP. Clues to finding correlates of risk/protection for HIV-1 vaccines [version 2; peer review: 2 approved with reservations] F1000 Research 2018, 6:868. https://doi.org/10.12688/f1000research.11818.2.
Schlom J, Jochems C, Gulley JL, Huang J. The role of soluble CD40L in immunosuppression. Oncoimmunology. 2013 Jan 1;2(1):e22546. doi: 10.4161/onci.22546.
Allen JE. IL-4 and IL-13: Regulators and Effectors of Wound Repair. Annu Rev Immunol. 2023 Apr 26;41:229-254. doi: 10.1146/annurev-immunol-101921-041206.
Pinto-Paz ME, Cotrina-Concha JM, Benites-Zapata VA. Mortality in cutaneous malignant melanoma and its association with Neutrophil-to-Lymphocyte ratio. Cancer Treat Res Commun. 2021;29:100464. doi: 10.1016/j.ctarc.2021.100464.
Matsushima K, Yang D, Oppenheim JJ. Interleukin-8: An evolving chemokine. Cytokine. 2022 May;153:155828. doi: 10.1016/j.cyto.2022.155828.
Chen Y, Jiang P, Wen J, Wu Z, Li J, Chen Y, Wang L, Gan D, Chen Y, Yang T, Lin M, Hu J. Integrated bioinformatics analysis of the crucial candidate genes and pathways associated with glucocorticoid resistance in acute lymphoblastic leukemia. Cancer Med. 2020 Apr;9(8):2918-2929. doi: 10.1002/cam4.2934.
Nelson AM, Zhao W, Gilliland KL, Zaenglein AL, Liu W, Thiboutot DM. Neutrophil gelatinase-associated lipocalin mediates 13-cis retinoic acid-induced apoptosis of human sebaceous gland cells. J Clin Invest. 2008 Apr;118(4):1468-78. doi: 10.1172/JCI33869.
Autio A, Nevalainen T, Mishra BH, Jylhä M, Flinck H, Hurme M. Effect of aging on the transcriptomic changes associated with the expression of the HERV-K (HML-2) provirus at 1q22. Immun Ageing. 2020 May 13;17:11. doi: 10.1186/s12979-020-00182-0.
Patterson BK, Yogendra R, Guevara-Coto J, Mora-Rodriguez RA, Osgood E, Bream J, Parikh P, Kreimer M, Jeffers D, Rutland C, Kaplan G, Zgoda M. Case series: Maraviroc and pravastatin as a therapeutic option to treat long COVID/Post-acute sequelae of COVID (PASC). Front Med (Lausanne). 2023 Feb 8;10:1122529. doi: 10.3389/fmed.2023.1122529.
Laderoute MP. A new paradigm about HERV-K102 particle production and blocked release to explain cortisol mediated immunosenescence and age-associated risk of chronic disease. Discov Med. 2015 Dec;20(112):379-91.
Laderoute M. The paradigm of immunosenescence in atherosclerosis-cardiovascular disease (ASCVD). Discov Med. 2020 Jan-Feb;29(156):41-51.
Laderoute M. Ivermectin may prevent and reverse immunosenescence by antagonizing alpha-fetoprotein and downmodulating PI3K/Akt/mTOR hyperactivity. Open Heart, April 29, 2021. https://openheart.bmj.com/content/8/1/e001655.responses#ivermectin-may-prevent-and-reverse-immunosenescence-by-antagonizing-alpha-fetoprotein-and-downmodulating-pi3k-akt-mtor-hyperactivity.
Ko JJ, Wu C, Mehta N, Wald-Dickler N, Yang W, Qiao R. A Comparison of Methylprednisolone and Dexamethasone in Intensive Care Patients With COVID-19. J Intensive Care Med. 2021 Jun;36(6):673-680. doi: 10.1177/0885066621994057.
Hong S, Wang H, Zhang Z, Qiao L. The roles of methylprednisolone treatment in patients with COVID-19: A systematic review and meta-analysis. Steroids. 2022 Jul;183:109022. doi: 10.1016/j.steroids.2022.109022.
Meduri GU, Chrousos GP. General Adaptation in Critical Illness: Glucocorticoid Receptor-alpha Master Regulator of Homeostatic Corrections. Front Endocrinol (Lausanne). 2020 Apr 22;11:161. doi: 10.3389/fendo.2020.00161.
Rajamohan T, Kurup PA. Lysine: arginine ratio of a protein influences cholesterol metabolism. Part 1--Studies on sesame protein having low lysine: arginine ratio. Indian J Exp Biol. 1997 Nov;35(11):1218-23.
Chacin-Bonilla, L. and Bonilla, E. 2023. Melatonin and Covid-19: An opened Pandora’s box and the hope for the time being. Melatonin Research. 6, 4 (Dec. 2023), 474-484. DOI:https://doi.org/https://doi.org/10.32794/mr112500163.
Zimmerman, S. and Reiter, R. 2019. Melatonin and the Optics of the Human Body. Melatonin Research. 2, 1 (Feb. 2019), 138-160. DOI:https://doi.org/https://doi.org/10.32794/mr11250016.
Chuffa, L., Carvalho, R., Camargo, V.L., Cury, S., Domeniconi, R., Zuccari, D.A. and Seiva, F.R. 2023. Melatonin and cancer: Exploring gene networks and functional categories. Melatonin Research. 6, 4 (Dec. 2023), 431-451. DOI:https://doi.org/https://doi.org/10.32794/mr112500161.
Patterson BK, Francisco EB, Yogendra R, Long E, Pise A, Rodrigues H, Hall E, Herrera M, Parikh P, Guevara-Coto J, Triche TJ, Scott P, Hekmati S, Maglinte D, Chang X, Mora-Rodríguez RA, Mora J. Persistence of SARS CoV-2 S1 Protein in CD16+ Monocytes in Post-Acute Sequelae of COVID-19 (PASC) up to 15 Months Post-Infection. Front Immunol. 2022 Jan 10;12:746021. doi: 10.3389/fimmu.2021.746021.
Kleen TO, Galdon AA, MacDonald AS, Dalgleish AG. Mitigating Coronavirus Induced Dysfunctional Immunity for At-Risk Populations in COVID-19: Trained Immunity, BCG and "New Old Friends". Front Immunol. 2020 Sep 4;11:2059. doi: 10.3389/fimmu.2020.02059.








Thank You, Dr. Laderoute, for reiterating that Vitamin-D is a currency of immune system economy, which we can readily provide, to keep our immune system functioning as designed. Some people, such as those who have had gallbladders removed, and many with a lot of body fat (into which vitamin-D diffuses) may need to take 10,000 units per day to get a mid-normal range blood level. Most people over 100# will be well served by 5000 units per day.
Checking a blood level after 3 months on a steady dose is a good idea.
Vitamin K2 seems to be synergistic with vitamin-D in many ways. I don't readily find study information on that, though. I personally take both.
If you read between the lines of this article [Barale C, Cavalot F, Frascaroli C, Bonomo K, Morotti A, Guerrasio A, Russo I. Association between High On-Aspirin Platelet Reactivity and Reduced Superoxide Dismutase Activity in Patients Affected by Type 2 Diabetes Mellitus or Primary Hypercholesterolemia. Int J Mol Sci. 2020 Jul 15;21(14):4983. doi: 10.3390/ijms21144983.] the induction of sCD40L by aspirin in familial hypercholesterolemia (FH) and in T2D seems to be blocked by statins. There should be a warning on the low dose aspirin where it currently says "Call 911, then chew 2 tablets (of aspirin 81 mg), if you think you are having a heart attack. Aspirin may help save your life." They need to add, use in patients with FH or T2D who are not on statin therapy may increase platelet activation (elevates sCD40L) which could worsen clotting and thus cardiovascular symptoms.